Women should be screened for breast cancer starting at age 40, 10 years earlier than recommended previously, a federal panel said on May 9.
The draft recommendation from the U.S. Preventive Services Task Force applies to most women and stems from a desire to detect breast cancer earlier.
“New and more inclusive science about breast cancer in people younger than 50 has enabled us to expand our prior recommendation and encourage all women to get screened every other year starting at age 40,” Dr. Carol Mangione, the previous chair of the task force, said in a statement. “This new recommendation will help save lives and prevent more women from dying due to breast cancer.”
The previous recommendation for women in their 40s was to decide on whether to get screened, and for all women to start at age 50 at the latest.
The panel now says women should get a mammogram at age 40 and thereafter every other year.
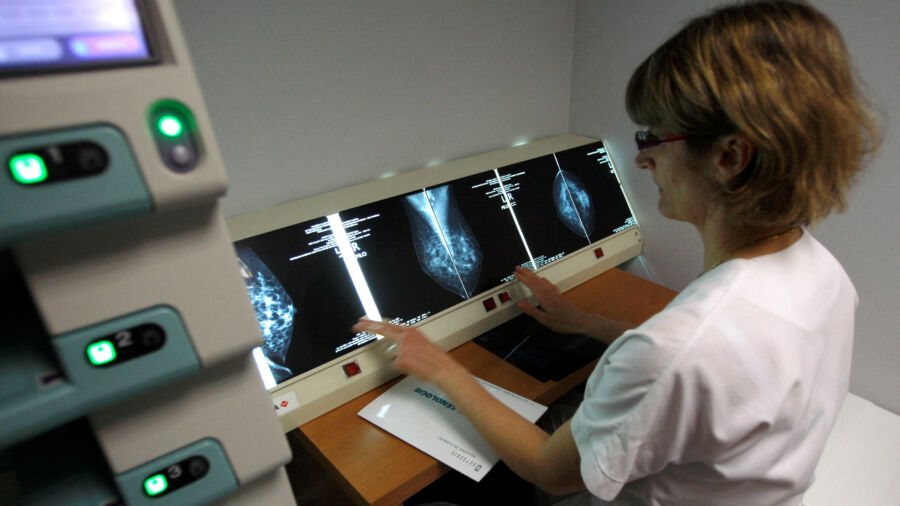
Mammograms are low-dose X-rays that image the breast. They are “the best primary screening tool to find breast cancer,” according to the U.S. Food and Drug Administration, and help to find many cancers before they are large enough to cause symptoms or pain.
The recommendation applies to women aged 40 to 74 deemed at average risk of breast cancer, including women who have a history of breast cancer in their family and woman with risk factors such as having dense breasts. It does not apply to women designated at very high risk of breast cancer because of certain genetic markers or women who have a history of breast cancer themselves.
The panel said that more research is needed to figure out how often women with dense breasts should get screened.
“We know that women with dense breasts are at higher risk of breast cancer and, unfortunately, mammograms do not work as well for them,” Dr. John Wong, a task force member, said in a statement. “What we don’t know yet, and what we are urgently calling for more research on, is whether and how additional screening for women with dense breasts might be helpful, including through ultrasound, breast MRIs, or something else.”
The draft recommendation will be available for public comment until June 5.
Change
The draft recommendation revises an earlier recommendation made by the panel in 2009, when it advised against routine mammograms for women in their 40s and said biennial screening should start at age 50, unless women and their doctors decided earlier screening was appropriate.
At that time, the net benefit of mammography screening for women in their 40s, minus the potential harms, was small, said Carol Mangione, who chairs the department of medicine at the David Geffen School of Medicine at the University of California.
“A lot of things have changed since then,” she said.
Breast cancer rates in younger women have been rising, digital mammography advances have improved their accuracy, and better treatments are resulting in improved survival, she said.
As a result, new computer models suggest that if biennial screening started at age 40 instead of age 50, and if everyone who is eligible got a mammogram, breast cancer mortality in the United States would be reduced by 20 percent, said Mangione.
The benefit would be even greater for black women, who generally have more aggressive breast cancers and poorer survival, the panel said.
Reactions
Groups largely said they support the proposed change from the U.S. Preventive Services Task Force (USPSTF).
“We applaud the return in USPSTF recommendations to begin screening in their 40s,” Dr. William Dahut, the American Cancer Society’s chief scientific officer.
The panel, though, should consider adjusting the recommended frequency of the screening. The society currently recommends women begin annual screening by age 45.
The American College of Radiology and Society of Breast Imaging also said that annual screenings should be recommended while all women should undergo a risk assessment by age 25 that could trigger an earlier start to mammograms.
The American College of Obstetricians and Gynecologists recommendations at present are to start at age 40, with additional mammograms annually or biannually
A U.S. woman’s lifetime risk of developing breast cancer in her lifetime is 12 percent, cancer groups say. The American Cancer Society estimates about 43,700 women will die from breast cancer this year, although the survival rate has increased over time, and millions of women with breast cancer live in the United States.
Older Women
USPSTF experts say there’s not enough evidence at present to recommend mammograms for women aged 75 or older.
“The balance of benefits and harms may shift as women age, but there is very limited research on this age population,” the panel said.
But the American Cancer Society recommends women continue to get screened, provided they are healthy and expected to live at least 10 more years.
“At the age of 75, the median life expectancy is greater than ten years, and many women 75 and older will be active and in good health for many more years,” Dahut said. “Because approximately one in four breast cancer deaths each year is attributable to a diagnosis after age 75, there is no reason to believe that the benefits that are evident in older women before age 74 would not carry forward with increasing age, not only preventing breast cancer deaths but avoiding suffering in the last years of life from aggressive therapy for advanced breast cancer.”
The Society of Breast Imaging and American College of Radiology also recommends women keep getting screened as they age, unless they have severe health issues that would curb their life expectancy.
Reuters contributed to this report.
From The Epoch Times