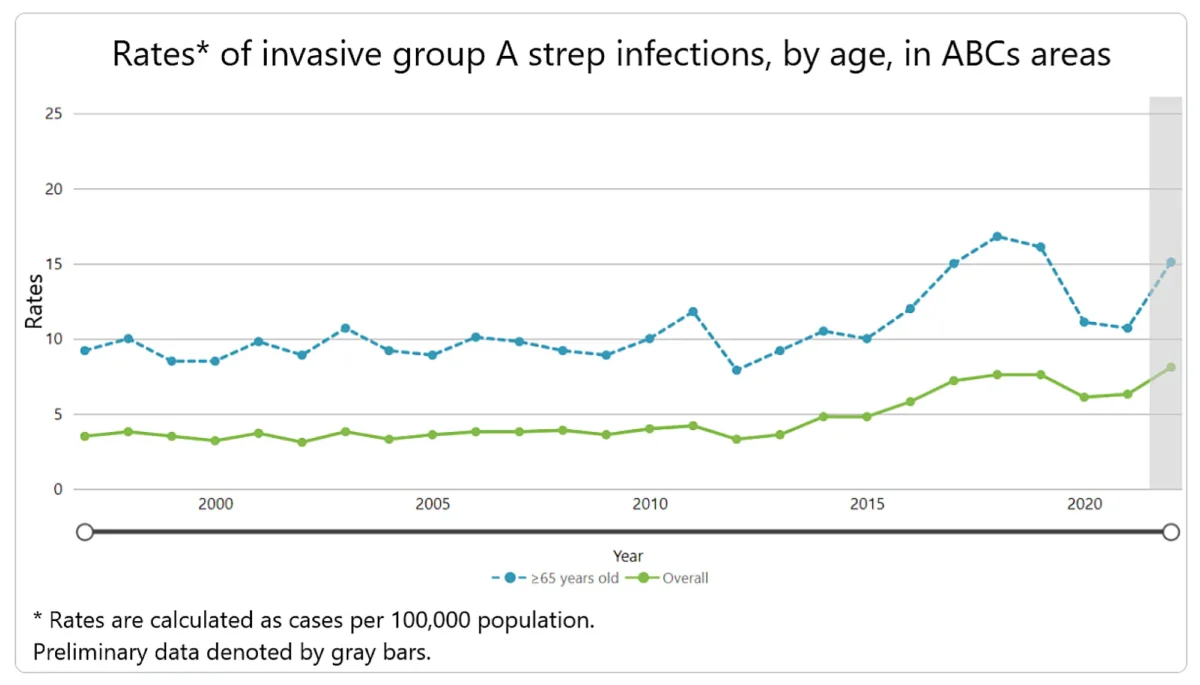
The number of invasive group A strep infections more than doubled from 2013 to 2022, a new study from the Centers for Disease Control and Prevention concluded, particularly among those 65 and older, while the bacteria also became more drug resistant.
Invasive group A streptococcus (GAS) infections occur when the bacteria, typically linked to mild illnesses like strep throat, invade parts of the body that are usually germ-free, such as the lungs or bloodstream.
When this happens, it can trigger life-threatening complications like necrotizing fasciitis—commonly known as flesh-eating disease—or streptococcal toxic shock syndrome, a severe immune response akin to sepsis, that can lead to organ failure.
The nine-year study, looking at a total of GAS 21,312 patients of whom 1,981 died, classified the incidences into three ages groups: aged 0 to 17 years who were 6 percent of the cases; aged 18-64 who were 64 percent of the cases; and 65 and older who were 30 percent of the cases. Though incidences remained highest among elderly patients, the relative increase over time was greatest among adults aged 18 to 64 years.
The authors attributed the increase, in part, to rising rates of diabetes and obesity, two conditions that weaken the immune system and can lead to skin infections.
In addition, “people experiencing homelessness, people who inject drugs, and residents of long-term care facilities had substantially elevated GAS incidence rates,” the authors said.
The study also highlighted that among the sampled GAS strains, the number that were resistant to macrolides and clindamycin—two widely used antibiotics—increased enormously, going up from 13 percent in 2013 to 33 percent in 2022—that is, a third of all GAS strains have now potentially become resistant to the most common groups of antibiotics.
The authors of the study called for “accelerated efforts” to prevent and control GAS infections, especially among groups at highest risk of infection.

