The report examined 23 million infections reported across 104 nations and analyzed microbial resistance to 22 antibiotics used for treating eight common bacterial pathogens responsible for four types of infections—bloodstream, urinary tract, gastrointestinal, and urogenital gonorrhea.
“In 2023, approximately one in six laboratory-confirmed bacterial infections worldwide were caused by bacteria resistant to antibiotics,” said the report.
“Trends in AMR indicate an increasing threat from Gram-negative bacterial pathogens.”
AMR was found to have increased in 40 percent of pathogen-antibiotic combinations between 2018 and 2023, according to the report. Annual increases were determined to be between 5 and 15 percent.
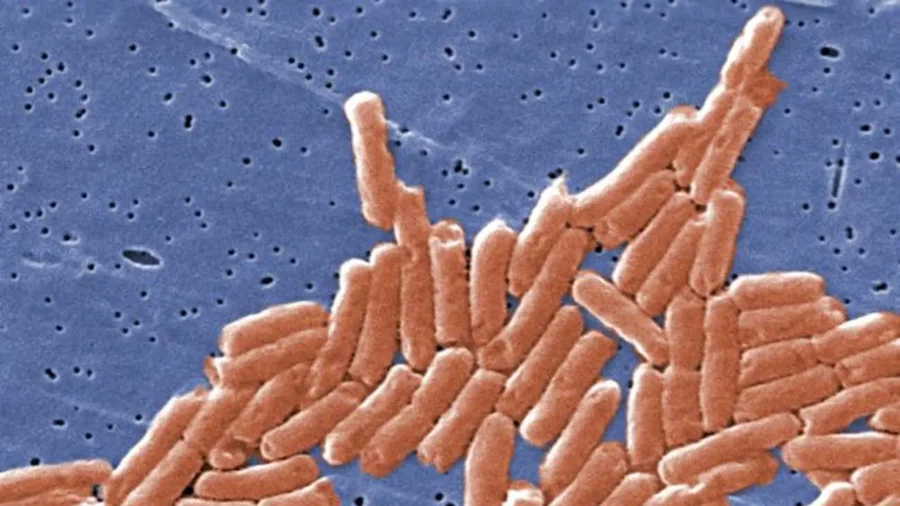
Resistance to certain antibiotics, particularly carbapenems and fluoroquinolones, was observed to be increasing among key Gram-negative pathogens, including E. coli, K. pneumoniae, and Salmonella, said the report.
“This is a concern, as these antibiotics are essential for the treatment of severe infections,” the report said.
K. pneumoniae, normally found in human stool, can cause bloodstream infections, pneumonia, meningitis, or surgical site infections, the CDC said.
Salmonella is considered to be the leading cause of foodborne illnesses and deaths in the United States, according to the agency.
Among the three leading Gram-negative pathogens that are responsible for serious bloodstream infections—E. coli, K. pneumoniae, and Acinetobacter—the frequency of resistance to carbapenems was found to be rising.
Acinetobacter, typically found in health care settings, can cause infections in the blood, lungs, wounds, and the urinary tract, according to the CDC.
K. pneumoniae and Acinetobacter, which are resistant to carbapenems, are linked with high fatality, exceeding 30 percent among infected individuals, the report said.
E. coli, resistant to third-generation antibiotic cephalosporin, was found to have a high incidence and morbidity, with more than 10,000 cases and 1.5 years lived with disability per million population.
Low Treatability, US-EU Alerts
The WHO report warned that the treatability of many of these antibiotic-resistant pathogens was “low to moderately low.”“Prevention of these infections is often difficult,” it said.
“Meanwhile, the antibiotic development pipeline remains weak and is unlikely to deliver effective alternatives in the near future for several of the most pressing threats.”
Antimicrobial resistance was less frequent in the European regions, with one in 10 infections being AMR, according to the WHO. It was least frequent in the Western Pacific region, at one in 11 infections.
AMR was identified to be most frequent in Southeast Asia and the Eastern Mediterranean regions, where almost one in three infections is categorized as such. This was followed by the African region, with one in five infections being AMR.
“As countries strengthen their AMR surveillance systems, we must use antibiotics responsibly, and make sure everyone has access to the right medicines, quality-assured diagnostics, and vaccines. Our future also depends on strengthening systems to prevent, diagnose, and treat infections and on innovating with next-generation antibiotics and rapid point-of-care molecular tests.”
Multiple global health agencies have issued alerts about AMR infections over the past weeks.