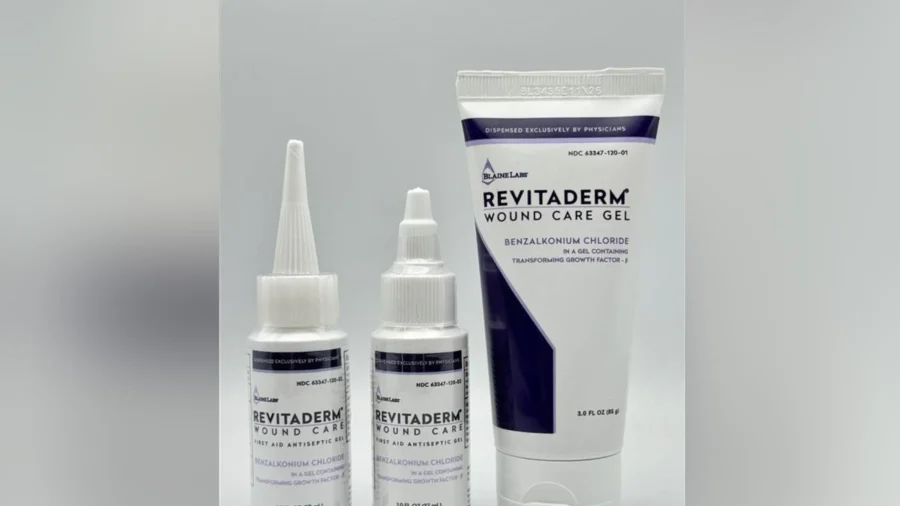
California-based Blaine Labs Inc. is recalling three lots of wound care gel products due to contamination with Lysinibacillus fusiformis bacteria.
Products impacted by the recall are 1 oz. and 3 oz. packages of “Revitaderm Wound Care Antiseptic Gel” and 1 oz. “Tridergel Wound Care,” the company said in an announcement published by the Food and Drug Administration on April 8. The products were distributed nationwide to health care providers.
Even though Lysinibacillus fusiformis is usually considered to have low pathogenicity in healthy people, it could act as an “opportunistic organism,” according to Blaine.
“Patients with open wounds, compromised skin barriers, or weakened immune systems (e.g., elderly, diabetic, or immunocompromised individuals) may be at increased risk for infection, skin irritation, and/or delayed wound healing,” the company said.
“In immunocompromised individuals, including those with poorly controlled diabetes, elderly individuals with immune senescence, and young children with an immature immune system, these infections may become severe and lead to life-threatening complications such as endocarditis or central system infection.”
The recalled Revitaderm items carry lot numbers BL3608 (expiry date: July 1, 2028), BL3435 (expiry date: Nov. 6, 2026), and BL3525 (expiry date: Aug. 7, 2027). For Tridergel, the lot number is BL3435, having an expiry date of Nov. 6, 2026.
According to the company, the products are used as antiseptics for first aid to help prevent infection in people who have suffered minor cuts, burns, and scrapes.
The voluntary recall was initiated after samples of the products tested positive for the bacteria. The company clarified that it has, to date, received no reports of adverse events linked to the recalled items.
“Customers & Healthcare providers should review their inventory for these affected lot numbers and discontinue use and/or distribution immediately,” the announcement said.
The Epoch Times reached out to Blaine Labs for comment but did not receive a response by publication time.
According to a June 2025 study published in the Pharmaceuticals journal, microbial contamination of drugs can have two key impacts: a reduction in the quality of drugs and a compromise in patient safety.
Changes in drug quality include alterations in its pharmaceutical form, such as the disintegration of tablets; breakdown of preservatives used in the medications, which can enable the growth of pathogens; and degradation of active substances used in the drugs.
The study called the degradation of preservatives and active substances two “distinct and harmful processes.”
Drug Contamination Risks
In July, the World Health Organization and the U.N. Office on Drugs and Crime released a report on contaminated medicines, finding that over the past nine decades, there were 25 documented cases of “excipient contamination” that resulted in more than 1,300 deaths globally. Excipients are inert substances used as vehicles for a drug.In the United States, the FDA alerts manufacturers about contaminated drugs. For instance, on July 24, the agency said it was alerting drug manufacturers about the risk of benzene contamination in drug components.
Benzene is a chemical used in the production of industrial products and known to be a human carcinogen, which refers to any substance that can cause cancer.
Lawmakers have taken action to improve accountability among manufacturers regarding drug safety.
Earlier this year, Sen. Rick Scott (R-Fla.) announced the Consumer Labeling for Enhanced API Reporting and Legitimate Accountability for Base Entity Listings (CLEAR LABELS) Act, which requires the country of origin to be included in drug labels, according to a Jan. 29 statement from the lawmaker’s office.
The senator said that many drugs are manufactured overseas, such as in China or India, with limited transparency and oversight over drug production, putting Americans at increased health risk.
“My CLEAR LABELS Act takes a commonsense approach to fix that by requiring clear disclosure of the original manufacturers of these drugs and their components, known as APIs,” Scott said.
“Transparency is critical to protecting patient safety, strengthening oversight, and reducing America’s overreliance on foreign drug production. Americans deserve to have confidence that the medicines they take are safe, regulated, and clearly labeled.”